What are Hemorrhoids
We all have Hemorrhoids! Hemorrhoids are a natural part of our anatomy, present from birth. They play an essential role in helping us control gas and stool. However, over time, they can become symptomatic and cause discomfort.
Hemorrhoids, also known as piles, are swollen veins in the lower rectum and anus. They affect a large portion of the population at some point in their lives. The duration of hemorrhoids varies depending on severity and lifestyle factors. Mild cases may resolve in a few days with proper care, while more severe cases might persist and require medical intervention.
Without treatment, symptomatic hemorrhoids can last from a few days to several weeks. Severe hemorrhoids are characterized by intense pain, significant bleeding, and constant discomfort. When a hemorrhoid bursts, it can cause sudden bleeding and pain, requiring immediate medical attention to prevent complications. Untreated hemorrhoids can lead to chronic pain, persistent bleeding, anemia, and even infections or abscesses. Internal hemorrhoids tend to bleed but are usually painless, while external hemorrhoids can be more painful and cause significant discomfort.
Symptoms
- Severe pain
- Intense itching
- Significant bleeding
- Internal hemorrhoids: Painless bleeding
- External hemorrhoids: Pain and swelling around the anus
- Itching
- Mild discomfort
- Small lumps around the anus
Causes
- Straining during bowel movements
- Chronic constipation or diarrhea
- Pregnancy
Mild cases can heal with proper care and lifestyle changes
- Managing mild symptoms is possible, but seeking treatment is recommended to avoid complications
Treatments
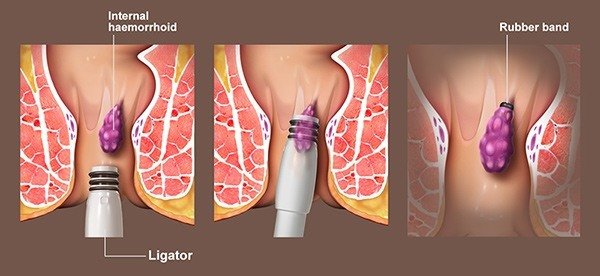
Rubber Band Ligation (RBL) is a minimally invasive Office-based procedure used to treat internal hemorrhoids. This procedure involves placing a small rubber band around the base of the hemorrhoid to cut off its blood supply. Without blood, the hemorrhoid shrinks and eventually falls off within a week.
RBL is most effective for treating internal hemorrhoids, especially those that bleed. It is not typically used for external hemorrhoids due to the potential for pain and complications.
The recovery time for RBL is relatively short. Most patients can return to their normal activities the next day, although it is common to experience some discomfort for a few days following the procedure. Complete healing typically occurs within one to two weeks.

Transanal Hemorrhoidal Dearterialization (THD) is an advanced procedure designed to reduce the blood flow to the hemorrhoids, causing them to shrink. This is achieved using a Doppler ultrasound to locate the arteries supplying blood to the hemorrhoids, which are then tied off. THD is less invasive than traditional hemorrhoidectomy and aims to minimize pain and recovery time.
THD is mainly for treating internal hemorrhoids, making it a versatile option for patients with multiple internal hemorrhoids or severe cases.
The recovery time for THD is generally short. Most patients can resume normal activities within a few days, although complete recovery may take up to two weeks. Patients typically experience less pain compared to other surgical treatments.
Dr. Mansouri at Heritage Surgical Group utilizes a specialized local anesthetic during the Transanal Hemorrhoidal Dearterialization (THD) procedure. This innovative approach provides effective pain relief for two days following the procedure, significantly longer than the typical few hours with standard anesthetics. This advanced technique helps ensure a more comfortable and smoother recovery experience for patients.
Hemorrhoidectomy
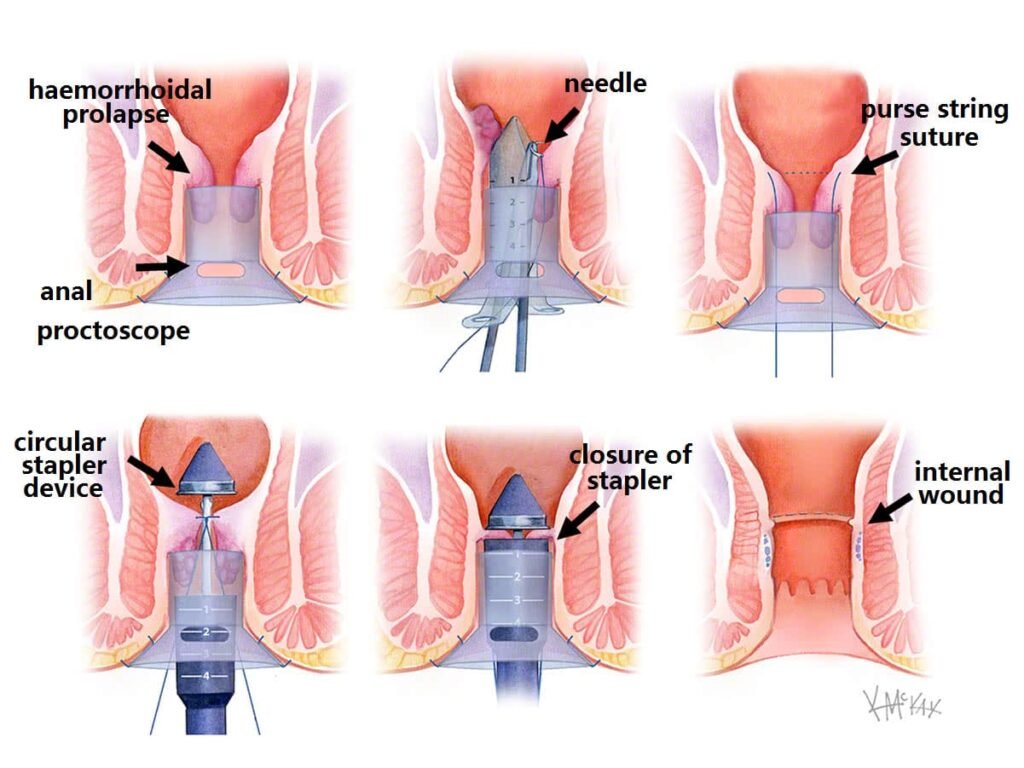
Hemorrhoidectomy is a surgical procedure for removing severe or recurrent hemorrhoids that do not respond to other treatments. This procedure involves the surgical excision of hemorrhoidal tissue.
Best Suited For: Hemorrhoidectomy is best suited for large, prolapsed, or thrombosed hemorrhoids and for patients who have not found relief from less invasive treatments.
The recovery time for hemorrhoidectomy is longer, typically ranging from two to four weeks. Patients may experience significant discomfort initially, but this decreases as healing progresses.
Dr. Mansouri at Heritage Surgical Group utilizes a specialized local anesthetic during the hemorrhoidectomy procedure, which significantly improves pain relief for two days, instead of just a few hours. This advanced pain management technique helps patients recover more comfortably.
Frequency Asked Questions
If you experience severe pain, heavy bleeding, or persistent symptoms that do not improve with home treatment, it is important to consult a doctor. Professional medical advice is also recommended if you notice a significant change in bowel habits or if a lump remains after a bowel movement.
Lying on your side or using a reclining chair can help reduce pressure on hemorrhoids. Using a donut-shaped cushion while sitting can also provide relief by alleviating pressure on the affected area.
It's best to avoid touching hemorrhoids to prevent irritation and potential infection. If you need to examine the area, make sure your hands are clean and use a gentle touch.
This may indicate a prolapsed hemorrhoid, which occurs when an internal hemorrhoid protrudes through the anus. It is advisable to consult a healthcare provider for appropriate treatment options.
Yes, you can have a colonoscopy if you have hemorrhoids. However, it is important to inform your doctor about your condition so they can take necessary precautions during the procedure.
Conditions such as anal fissures, abscesses, skin tags, and certain types of growths can resemble external hemorrhoids. Proper diagnosis by a healthcare provider is essential to ensure appropriate treatment.
To minimize pain and strain during bowel movements, consider using a stool to elevate your feet, which can help align the rectum and make passing stools easier. Avoid straining and take your time to prevent exacerbating the hemorrhoids.
Hemorrhoids cause swelling and lumps, while anal fissures result in sharp pain and bleeding. Fissures are small tears in the lining of the anus, whereas hemorrhoids are swollen veins. A healthcare provider can help diagnose the condition accurately.
Yes, it is possible to have both conditions simultaneously. Proper diagnosis and treatment from a healthcare provider are necessary to manage both issues effectively.