- POWERFUL SURGICAL SOLUTIONS FOR YOUR HEALTH
- Phone: (201) 833-2888


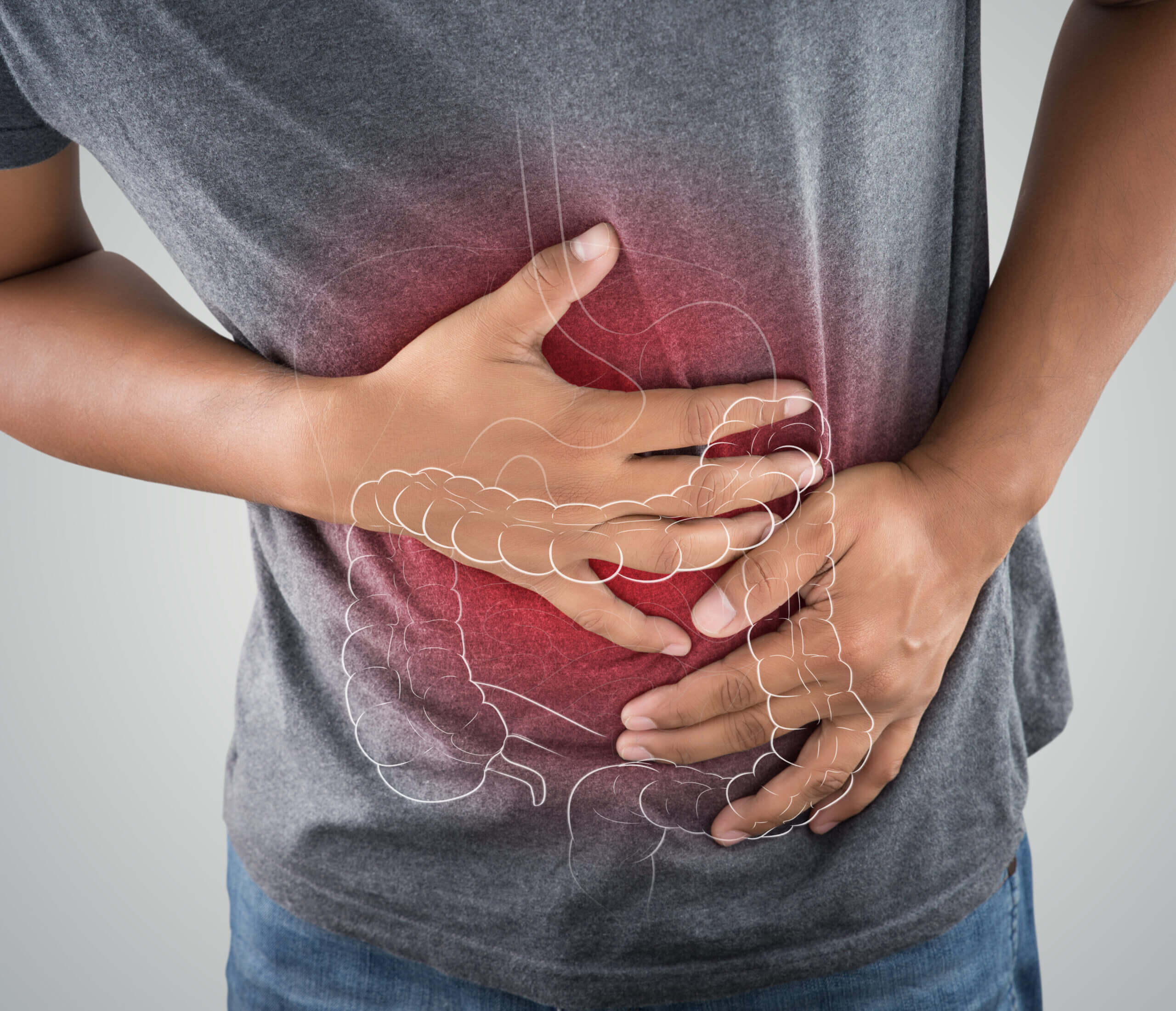
Typically, prior to surgery, the colon may be evaluated with colonoscopy and/or imaging, to make a diagnosis of a benign or malignant disorder. In cases of malignancy, or benign colonic disorders which have failed medical management, patients may require colon resection for treatment or cure.
The majority of patients tolerate partial colon resection with minimal physiologic consequences. Minor consequences are related to fluid absorption, which include temporary loose stools which can be managed medically with increased fiber and anti-motility agents until the body adapts. This may be more pronounced with larger resections. Laparoscopic colon resection is associated with lower rates of wound infection, use of pain medication, and quicker return to daily living.
In a small subset of patients, a colostomy may be required as a safety precaution, to allow the intestines and abdominal cavity to heal prior to reversing the colostomy and reconnecting the colon.
Much like a colonoscopy, the bowel will need to be cleaned out prior to surgery to help reduce the rate of wound and abdominal infections. A mechanical bowel prep (ex. Golytly) combined with oral antibiotics is given the day before surgery in combination with intravenous antibiotics on the day of surgery to improve outcomes.
After colon surgery, patients are typically in the hospital for 3-4 days waiting for return of bowel function and diet is tolerated. Patients are encouraged to be up and walking right after surgery. Pain control with narcotic pain medication may be indicated, but should be taken with a stool softener to prevent constipation. Follow up is typically surgeon specific, and specific to the indication for surgery. Long term, patients are encouraged to maintain a high fiber diet for colon health.

Typically, prior to surgery, the colon may be evaluated with colonoscopy and/or imaging, to make a diagnosis of a benign or malignant disorder. In cases of malignancy, or benign colonic disorders which have failed medical management, patients may require colon resection for treatment or cure.
The majority of patients tolerate partial colon resection with minimal physiologic consequences. Minor consequences are related to fluid absorption, which include temporary loose stools which can be managed medically with increased fiber and anti-motility agents until the body adapts. This may be more pronounced with larger resections. Laparoscopic colon resection is associated with lower rates of wound infection, use of pain medication, and quicker return to daily living.
In a small subset of patients, a colostomy may be required as a safety precaution, to allow the intestines and abdominal cavity to heal prior to reversing the colostomy and reconnecting the colon.
Much like a colonoscopy, the bowel will need to be prepped and cleaned out prior to surgery to help reduce the rate of wound and abdominal infections. A mechanical bowel prep (ex. Golytly) combined with oral antibiotics is given the day before surgery in combination with intravenous antibiotics on the day of surgery to improve outcomes.

After colon surgery, patients are typically in the hospital for 3-4 days waiting for return of bowel function and diet is tolerated. Patients are encouraged to be up and walking right after surgery. Pain control with narcotic pain medication may be indicated, but should be taken with a stool softener to prevent constipation. Follow up is typically surgeon specific, and specific to the indication for surgery. Long term, patients are encouraged to maintain a high fiber diet for colon health.
Typically, prior to surgery, the colon may be evaluated with colonoscopy and/or imaging, to make a diagnosis of a benign or malignant disorder. In cases of malignancy, or benign colonic disorders which have failed medical management, patients may require colon resection for treatment or cure.
Wound care instructions and pain medication will be provided by your surgeon
The majority of patients tolerate partial colon resection with minimal physiologic consequences. Minor consequences are related to fluid absorption, which include temporary loose stools which can be managed medically with increased fiber and anti-motility agents until the body adapts. This may be more pronounced with larger resections. Laparoscopic colon resection is associated with lower rates of wound infection, use of pain medication, and quicker return to daily living.
In a small subset of patients, a colostomy may be required as a safety precaution, to allow the intestines and abdominal cavity to heal prior to reversing the colostomy and reconnecting the colon.
Much like a colonoscopy, the bowel will need to be cleaned out prior to surgery to help reduce the rate of wound and abdominal infections. A mechanical bowel prep (ex. Golytly) combined with oral antibiotics is given the day before surgery in combination with intravenous antibiotics on the day of surgery to improve outcomes.
After colon surgery, patients are typically in the hospital for 3-4 days waiting for return of bowel function and diet is tolerated. Patients are encouraged to be up and walking right after surgery. Pain control with narcotic pain medication may be indicated, but should be taken with a stool softener to prevent constipation. Follow up is typically surgeon specific, and specific to the indication for surgery. Long term, patients are encouraged to maintain a high fiber diet for colon health.
Ready to get started?
Visit any of our convenient locations in Bergen Country or fill out the form to contact us today!
Our surgeons offer comprehensive surgical solutions and specialize in laparoscopic and robotic, minimally invasive surgery, which means less pain, shorter hospital stay, and quicker recovery time, so you can get back to your daily life.

Copyright 2024 by Heritage Surgical Group. All rights reserved.